Comprehensive Exploration of the Inner Ear Anatomy
Exploring the Structure and Essential Functions of the Cochlea
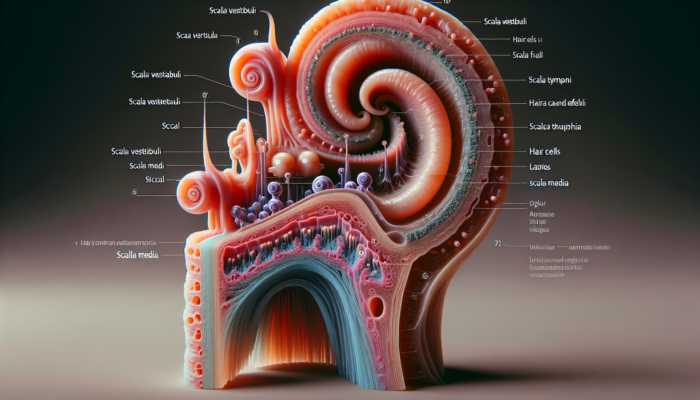
The cochlea represents an extraordinary spiral-shaped organ located within the inner ear, integral to our capacity to perceive sound. This complex structure is responsible for converting sound vibrations into electrical signals, which are subsequently relayed to the brain for interpretation. This conversion process is crucial for us to enjoy and understand the intricate layers of sound. The cochlea is divided into three main chambers: the scala vestibuli, scala tympani, and scala media, each containing fluid and lined with specialised hair cells that respond to sound waves. As sound enters the cochlea, it generates pressure waves that travel through these fluids, bending the hair cells and producing electrical impulses that are transmitted to the auditory nerve for processing.
A thorough understanding of cochlear anatomy not only underscores its essential functions, but also highlights its susceptibility to damage. The delicate hair cells within the cochlea are vulnerable to numerous factors, including aging, prolonged exposure to loud sounds, and certain medical conditions, which can lead to hearing loss. Research indicates that exposure to noise levels exceeding 85 decibels can result in noise-induced hearing loss, a widespread risk encountered in diverse environments worldwide, from concerts to bustling urban streets. Therefore, raising awareness about safe listening practices is crucial for preserving cochlear health, enabling individuals globally to appreciate the rich soundscapes that life has to offer.
Exploring the Vestibular System’s Essential Contribution to Balance
The vestibular system, located within the inner ear, plays a fundamental role in maintaining balance and spatial orientation. This intricate system comprises complex structures, primarily the semicircular canals and otolith organs, which work in unison to detect head movements and shifts in body position. The semicircular canals are specifically designed to sense angular motion, while the otolith organs excel at detecting linear movements and the effects of gravity. The information supplied by these structures is crucial for everyday activities, encompassing everything from walking and running to more complex movements such as dancing or engaging in sports.
The global significance of the vestibular system is evident in various contexts. For instance, athletes involved in disciplines such as gymnastics or figure skating heavily depend on their vestibular sense to maintain balance and execute precise movements. Likewise, individuals residing in areas characterised by diverse terrains, like mountainous regions, must navigate challenging landscapes, making a well-functioning vestibular system vital for safety and mobility. Disorders affecting this system can lead to symptoms such as dizziness or imbalance, which can severely impact an individual’s quality of life and daily activities.
Investigating the Auditory Nerve’s Crucial Role in Sound Transmission
The auditory nerve serves as a vital pathway for transmitting sound information, transferring electrical signals from the cochlea to the brain, where these signals are deciphered as sound. This nerve constitutes a fundamental component of the central nervous system, facilitating the complex experience of hearing. The seamless connection between the cochlea and the auditory cortex ensures that even the most intricate auditory experiences—ranging from a symphony to the gentle rustling of leaves or the voice of a cherished friend—are perceived with clarity and precision.
However, various conditions affecting the auditory nerve can lead to significant challenges, including hearing loss and auditory processing disorders. Individuals across the globe face numerous risks to their auditory health, from exposure to industrial noise in urban environments to untreated ear infections in rural settings. Recent advancements in medical technology, such as the development of cochlear implants, represent groundbreaking solutions for individuals suffering from severe hearing impairments, allowing them to reconnect with the auditory world in transformative ways that were once deemed impossible.
In-Depth Review of the Anatomy of the Outer Ear
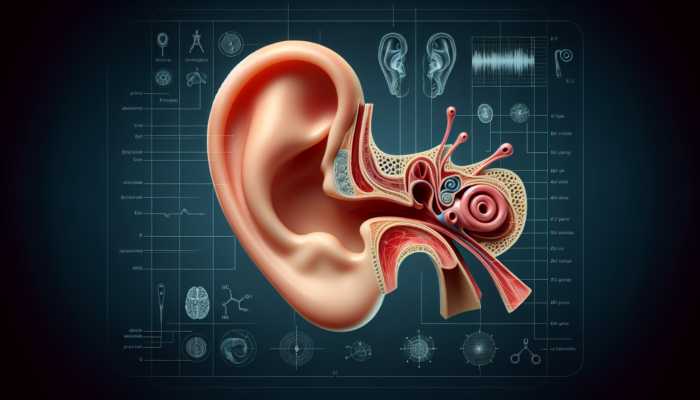
Exploring the Pinna’s Key Role in Capturing Sound Waves
The pinna, also known as the auricle, constitutes the outermost section of the ear, fulfilling a crucial function in capturing sound waves from the surrounding environment. Its distinctive shape acts as a funnel, directing sound waves into the ear canal. The unique contours and folds of the pinna not only facilitate effective sound collection but also enhance our ability to discern the direction of sounds, which is a vital aspect of auditory perception.
Globally, the anatomical design of the pinna displays variations across different populations, shaped by evolutionary and environmental influences. For example, individuals inhabiting densely wooded regions may exhibit slightly different ear shapes compared to those from open plains. These adaptations illustrate the intricate relationship between anatomy and environmental factors, underscoring the importance of understanding such variations within fields like anthropology and audiology. Furthermore, congenital ear deformities can significantly impact sound collection and localisation, emphasising the need for tailored auditory solutions on a global scale.
Examining the Structure and Function of the Ear Canal
The ear canal is a tubular structure that extends from the pinna to the eardrum, playing a pivotal role in transmitting sound. This passage not only channels sound waves but also amplifies them before they reach the eardrum, thereby enhancing auditory perception. The unique shape and length of the ear canal are specifically designed to optimise sound amplification, ensuring that even the quietest sounds are effectively detected.
An intriguing aspect of the ear canal’s structure is its protective function. The canal is lined with skin that produces cerumen, commonly referred to as earwax, which serves multiple purposes: trapping dust, debris, and microorganisms while providing a barrier against infections. Globally, earwax impaction is a common concern, with individuals from diverse backgrounds experiencing discomfort and temporary hearing loss as a result. Awareness campaigns promoting ear health and proper cleaning techniques can help alleviate these issues, ensuring that the ear canal remains an effective conduit for sound transmission.
Understanding the Vital Role of the Eardrum in Sound Transmission
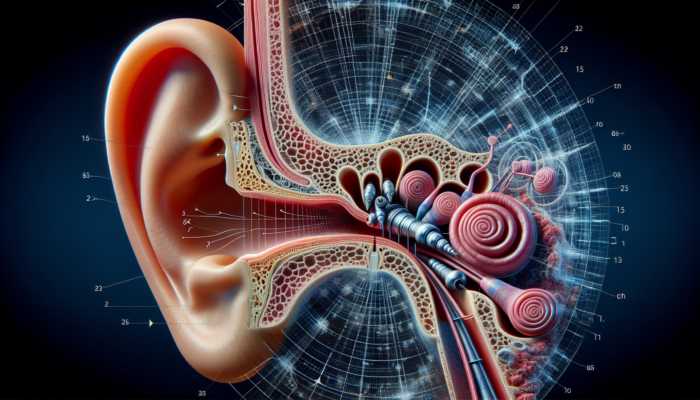
The eardrum, referred to as the tympanic membrane, is a thin yet robust structure that vibrates in response to sound waves. This vibration is essential, as it translates acoustic energy into mechanical energy, which is subsequently conveyed to the middle ear. The eardrum’s sensitivity is remarkable, capable of responding to a wide range of frequencies, enabling us to perceive sounds that span from a mere whisper to the powerful crescendo of a concert.
Globally, the health of the eardrum is paramount; various factors such as exposure to loud sounds, ear infections, and physical trauma can compromise its integrity. For instance, barotrauma—which occurs due to sudden pressure changes during air travel—can lead to eardrum perforation, resulting in pain and hearing loss. Awareness and preventive measures, such as using earplugs during flights or swimming, are crucial for safeguarding this vital component of hearing. The eardrum’s role in sound transmission is critical, acting as the gateway to the middle ear and beyond.
Investigating the Intricate Anatomy of the Pinna
The anatomy of the pinna is intricate, primarily composed of cartilage surrounded by skin. Its distinctive shape, characterised by various folds and depressions, significantly aids in sound localisation and collection. These anatomical features enhance our ability to differentiate between sounds originating from different directions, a skill that is essential for survival and social interaction within our environment.
This anatomical diversity is particularly fascinating when examining populations worldwide. Certain cultural groups may have developed unique modifications to the pinna for aesthetic purposes or to enhance auditory capabilities in specific contexts. Additionally, congenital deformities of the pinna can impact sound perception, leading to a deeper understanding of how ear anatomy correlates with hearing ability. This knowledge proves invaluable for creating effective interventions for auditory impairments, ensuring that individuals can fully engage with their auditory environments.
Understanding the Protective Features of the Ear Canal
The design of the ear canal serves not only to transmit sound but also to provide a protective barrier against foreign objects and debris. The skin lining the ear canal produces earwax, which acts as a natural defence mechanism. This substance traps dust, foreign particles, and microorganisms, preventing them from reaching the eardrum and reducing the likelihood of infections. Furthermore, earwax aids in keeping the skin of the ear canal moisturised, preventing dryness and irritation.
Globally, earwax impaction is a widespread issue affecting many individuals. Excessive wax build-up can lead to discomfort, reduced hearing, and even tinnitus. Education on ear hygiene practices, such as avoiding cotton swabs that can push wax deeper into the canal, is crucial. Moreover, understanding cultural practices related to ear care can inform health interventions. Recognising the balance between natural ear protection and the necessity for hygiene is essential for maintaining auditory health across the globe.
Key Functions of the Inner Ear
How the Hearing Mechanism Transforms Sound Waves
The core function of the inner ear revolves around the intricate hearing mechanism that converts mechanical sound waves into electrical signals. This process begins when sound waves enter the cochlea, inducing fluid movements. These movements are critical for bending the hair cells situated along the basilar membrane within the cochlea. As these hair cells bend, they generate electrical impulses that travel through the auditory nerve to the brain, where they are decoded as distinct sounds.
The efficiency of this hearing mechanism is paramount for effective communication and interaction across various settings, whether one is enjoying music in a concert hall or engaging in conversation within a bustling café. Variations in hearing ability among individuals can stem from genetic factors, exposure to environmental noise, or lifestyle choices, each influencing how sound is perceived. Globally, numerous individuals experience hearing impairments that can affect their social lives and professional opportunities, emphasising the need for accessible hearing health services and education.
The Vestibular System’s Fundamental Role in Balance and Equilibrium
The vestibular system within the inner ear is a marvel of anatomical engineering, playing a crucial role in maintaining balance and equilibrium. By continuously monitoring head position and movement through the semicircular canals and otolith organs, this system provides the brain with essential information for sustaining stability. When we turn our heads or move our bodies, the fluid within these canals shifts, stimulating hair cells that send signals to the brain about our orientation in space.
This ability to maintain balance is not only essential for athletes or dancers; everyday activities such as walking, climbing stairs, or even standing still rely heavily on our vestibular system. Globally, individuals engaged in occupations requiring physical agility—ranging from construction workers to dancers—must possess a keen sense of balance to perform their tasks safely. Furthermore, conditions like vertigo or vestibular disorders can severely disrupt this function, underscoring the need for global awareness and understanding of vestibular health.
Sound Localization: The Mechanism Behind Determining Direction and Source
An often-overlooked function of the inner ear is its role in sound localization. The inner ear assists in determining the direction and source of sounds by analysing the differences in timing and intensity of sound waves that reach each ear. This capability is critical for navigating our environments, allowing us to respond swiftly to auditory cues.
For instance, in a busy street, the ability to pinpoint the sound of a honking car or a friend calling from behind greatly enhances our spatial awareness and safety. This function is even more pronounced in the animal kingdom, where certain species can locate prey or predators using advanced auditory skills. Globally, understanding sound localization can inform technologies such as hearing aids and sound systems, enriching the auditory experience for individuals with hearing impairments.
Examining the Functions of the Outer Ear
The Essential Function of Sound Collection in Hearing
The primary function of the outer ear lies in collecting and funneling sound waves into the ear canal. This collection process commences with the pinna, which captures sound from various directions and directs it toward the ear canal. The design and shape of the pinna are optimised for enhanced sound collection, maximising our hearing capabilities, particularly in environments filled with competing sounds.
In diverse locations around the globe, the significance of sound collection extends beyond human communication; it is also critical in wildlife communication and survival. For instance, many animals depend on their outer ear structures to detect environmental sounds—whether it be a predator approaching or their mate calling. The evolutionary adaptations in ear shapes across different species illustrate the importance of sound collection in various ecological niches, further emphasising the interconnectedness of auditory health.
The Mechanism of Sound Amplification in the Outer Ear
Sound amplification is a vital function of the outer ear, where the unique configuration of the ear canal enhances the volume of sound waves before they reach the eardrum. This amplification allows even the faintest sounds to become audible, contributing to our rich auditory experiences. The ear canal functions like a resonator, boosting specific frequencies of sound, thereby facilitating the perception of speech or musical notes.
In various cultures, the ability to hear well is often celebrated, from traditional music to oral storytelling, reflecting the deep-rooted significance of sound amplification in social interactions. Understanding how sound amplification operates can also inform the design of hearing aids and other auditory technologies. For individuals with hearing impairments, grasping the mechanics of sound amplification can lead to better management of their auditory health.
The Protective Functions of the Outer Ear Against Debris
The outer ear, including the ear canal, acts as a protective barrier against foreign objects and debris entering the ear. The skin lining the ear canal produces earwax, which traps dust, debris, and microorganisms, preventing them from reaching the delicate structures deeper within the ear. This natural defence mechanism is essential for maintaining ear health and preventing infections.
Globally, awareness of ear protection is crucial, particularly in environments with high levels of dust, pollution, or water exposure, such as during swimming. Engaging in preventive measures, such as using earplugs in noisy environments or maintaining proper ear hygiene, can help individuals sustain healthy ears. Understanding the protective functions of the outer ear encourages people worldwide to prioritise ear health and take proactive measures against potential auditory threats.
The Role of the Outer Ear in Sound Localization
The outer ear also plays a significant role in sound localization, aiding in the determination of the source and direction of sounds. The shape of the pinna, combined with the timing and intensity of sounds reaching each ear, allows us to accurately locate where a sound originates—an essential skill for survival and interaction in our environment.
This ability is particularly evident across various global contexts, such as in urban environments where discerning sounds is vital for safety. For example, recognising the direction of approaching emergency vehicles or identifying familiar voices in crowded spaces relies on effective sound localization. Enhancing our understanding of sound localization can also improve auditory technologies, enriching experiences for individuals with hearing impairments and contributing to safer environments overall.
Common Disorders Impacting the Inner Ear
Understanding the Mechanisms Behind Sensorineural Hearing Loss
Sensorineural hearing loss is a prevalent condition that arises from damage to the hair cells of the inner ear or the auditory nerve. This type of hearing loss commonly manifests as difficulty in hearing soft sounds or distinguishing speech amidst background noise. Various factors contribute to sensorineural hearing loss, including the natural process of aging, exposure to loud sounds, and certain medical conditions, such as ototoxicity resulting from specific medications.
Globally, this condition affects millions, creating barriers to effective communication and social interactions. Awareness initiatives aimed at promoting hearing protection in noisy environments, such as concerts or industrial workplaces, are crucial in preventing this type of hearing loss. Additionally, advancements in hearing aids and cochlear implants offer individuals experiencing sensorineural hearing loss opportunities to regain access to sound, underscoring the ongoing need for innovation in auditory healthcare.
Exploring the Complexities of Ménière’s Disease
Ménière’s disease is a complex inner ear disorder characterised by episodes of vertigo, hearing loss, and tinnitus. This condition is thought to be related to fluid accumulation in the inner ear, which disrupts both balance and hearing. The unpredictable nature of Ménière’s disease can significantly affect an individual’s quality of life, often leading to anxiety and social withdrawal.
Globally, raising awareness and understanding of Ménière’s disease is vital for effective diagnosis and management. Educational initiatives can assist individuals in recognising symptoms early and prompt them to seek medical attention. Treatment options vary, ranging from lifestyle adjustments and dietary changes to medical interventions, highlighting the importance of personalised care strategies for managing this condition and enhancing overall well-being.
Vestibular Neuritis: Causes, Symptoms, and Effects
Vestibular neuritis is an inner ear disorder marked by sudden and intense vertigo resulting from inflammation of the vestibular nerve. This condition frequently follows a viral infection and can cause significant disruptions in balance and spatial awareness. Individuals may experience severe spinning sensations, nausea, and difficulties in performing daily activities.
Globally, vestibular neuritis highlights the intricate connection between viral infections and inner ear health. Understanding this correlation can inform public health initiatives aimed at preventing viral illnesses and their potential complications. While vestibular neuritis is typically self-limiting, targeted rehabilitation therapy can support individuals in regaining their balance and minimising the long-term impact on their daily lives.
Common Disorders Affecting the Outer Ear
Understanding Otitis Externa: The Reality of Swimmer’s Ear
Otitis externa, commonly referred to as swimmer’s ear, denotes an infection or inflammation of the outer ear canal. This condition often arises when water becomes trapped in the ear after swimming, creating an environment conducive to bacterial growth. Symptoms may include itching, redness, and pain, leading to discomfort for those affected.
Globally, otitis externa is prevalent among swimmers and individuals involved in water sports. Preventive measures, such as keeping the ears dry and using earplugs, can significantly reduce the risk of developing this condition. Moreover, awareness of proper ear hygiene practices is essential in minimising the occurrence of otitis externa and promoting overall ear health.
Earwax Impaction: Causes, Effects, and Solutions
Earwax impaction occurs when excessive earwax accumulates in the ear canal, resulting in blockage and potential hearing loss. While earwax serves a protective function, overproduction can lead to discomfort, tinnitus, and difficulties in hearing. Factors contributing to earwax impaction include the use of cotton swabs, which can inadvertently push wax deeper into the canal.
Globally, earwax impaction is a common issue that affects individuals across various cultures. Education on proper ear hygiene practices, including avoiding cotton swabs and seeking professional cleaning when necessary, can help mitigate this problem. Understanding the balance between maintaining ear health and preventing impaction is crucial for all individuals.
Understanding Auricular Hematomas in Athletes
An auricular hematoma is a collection of blood between the cartilage and skin of the pinna, typically resulting from trauma or blunt force injury. This condition is particularly prevalent in contact sports, where athletes are at a heightened risk for ear injuries. If left untreated, auricular hematomas can lead to permanent deformities known as “cauliflower ear.”
Globally, awareness of auricular hematomas within athletic contexts is essential for injury prevention and ensuring proper treatment. Preventive measures, such as wearing protective headgear during contact sports, can significantly reduce the risk of developing auricular hematomas. Prompt medical intervention is crucial for managing this condition and preserving the aesthetic and functional integrity of the ear.
Exostoses and Osteomas: Understanding Benign Bone Growths in the Ear Canal
Exostoses are benign bone growths in the ear canal, often associated with prolonged exposure to cold water, while osteomas are similar growths that can obstruct the ear canal and impact hearing. Both conditions are more frequently observed in individuals who engage in water sports, particularly surfers and swimmers.
Globally, awareness and understanding of these conditions are essential for individuals participating in aquatic activities. Regular check-ups with healthcare professionals can facilitate early detection and treatment, preventing complications arising from exostoses and osteomas. Education on the importance of ear protection while swimming or surfing can be instrumental in preserving ear health for aquatic enthusiasts.
Diagnostic Approaches for Inner Ear Disorders
The Significance of Hearing Tests in Diagnosing Conditions
Hearing tests, such as audiometry, are essential diagnostic tools for evaluating inner ear disorders. These tests measure an individual’s ability to hear a range of frequencies and sound intensities, aiding in identifying the type and extent of hearing loss. Professionals administer these tests in controlled environments to ensure accurate results for effective diagnosis.
Globally, early detection through routine hearing tests is vital for addressing hearing impairments. Recognising the importance of regular hearing assessments can lead to timely interventions, enhancing overall auditory health. Recent advancements in telehealth technology have expanded access to hearing tests, enabling individuals in remote areas to obtain necessary evaluations.
Comprehensive Testing for Evaluating Balance
Balance tests, including vestibular function tests, assess the performance of the vestibular system within the inner ear. These tests measure how well the body maintains balance and reacts to changes in head position. Various protocols, such as posturography tests or caloric testing, help identify vestibular disorders that may contribute to dizziness and balance issues.
Globally, balance tests play an essential role in diagnosing conditions such as vestibular neuritis and Ménière’s disease. Awareness of the importance of balance assessments can prompt individuals experiencing dizziness to seek medical advice, leading to effective management strategies. With the increasing focus on balance-related health, particularly in the ageing population, these tests are increasingly vital for ensuring safe and active lifestyles.
Utilising Imaging Techniques for Accurate Diagnosis
Imaging techniques, such as MRI and CT scans, are invaluable for diagnosing complex inner ear disorders. These advanced imaging modalities enable healthcare professionals to visualise the structures of the inner ear, assisting in identifying abnormalities like tumours or malformations that may affect hearing and balance.
Globally, accessibility to imaging technologies has improved diagnostic accuracy and timely management of inner ear disorders. Awareness of available imaging options can motivate individuals to pursue comprehensive evaluations, facilitating effective treatment plans. As technology advances, the incorporation of imaging techniques into routine diagnostic protocols will enhance our understanding of inner ear health worldwide.
Endoscopy: A Minimally Invasive Diagnostic Method
Endoscopy is a minimally invasive diagnostic procedure employed to visualise the inner ear and evaluate its structures. This technique allows healthcare professionals to directly examine the ear canal and eardrum, enabling accurate diagnosis and treatment of various conditions.
Globally, the use of endoscopic techniques in ear examinations has increased, improving patient outcomes through comprehensive assessments. Understanding the advantages of endoscopy can empower individuals to seek timely medical intervention for ear-related concerns. As technological advancements continue, endoscopy may play a pivotal role in the future of ear health diagnostics and management.
The Significance of Genetic Testing in Understanding Inner Ear Disorders
Genetic testing is an emerging diagnostic tool aimed at understanding hereditary inner ear disorders. By identifying genetic mutations linked to conditions such as Usher syndrome or otosclerosis, healthcare professionals can offer more personalised care and management strategies for affected individuals and their families.
Globally, integrating genetic testing into healthcare systems can enhance our understanding of the genetic basis of hearing loss and inform treatment options. Raising awareness about the availability of genetic testing may encourage individuals with a family history of hearing disorders to pursue evaluations, paving the way for targeted interventions and improved outcomes.
Frequently Asked Questions About Ear Health
What are the Distinctive Features of the Inner Ear Compared to the Outer Ear?
The inner ear is responsible for converting sound vibrations into electrical signals and for maintaining balance, while the outer ear functions to collect and funnel sound waves into the ear canal for amplification.
Do Disorders of the Inner Ear Affect Balance?
Yes, disorders impacting the inner ear, such as vestibular neuritis or Ménière’s disease, can significantly disrupt balance and spatial awareness, resulting in dizziness and instability.
What Function Does the Cochlea Serve in the Hearing Process?
The cochlea transforms sound vibrations into electrical signals through its intricate fluid-filled structure, allowing the brain to perceive sound accurately and distinctly.
How Does Earwax Play a Role in Ear Protection?
Earwax serves as a natural barrier, trapping dust, debris, and microorganisms, preventing them from reaching the eardrum and diminishing the risk of infections.
What Common Symptoms are Indicative of Sensorineural Hearing Loss?
Common symptoms include difficulty in hearing faint sounds, challenges in understanding speech in noisy settings, and a noticeable decline in sound clarity.
What Preventive Measures Can Be Taken to Avoid Otitis Externa?
To prevent otitis externa, it is crucial to keep ears dry after swimming, avoid inserting objects into the ear canal, and use earplugs when swimming in potentially contaminated water.
Why is Sound Localization Important for Individuals?
Sound localization is vital for spatial awareness, enabling individuals to determine the source and direction of sounds, which is essential for safety and social interaction.
How Can Vestibular Disorders Be Managed Effectively?
Vestibular disorders may be treated through physical therapy, medications, or lifestyle changes aimed at alleviating symptoms and restoring balance.
When is it Necessary to Seek Medical Attention for Ear-Related Issues?
Seek medical attention if you experience persistent pain, hearing loss, dizziness, or any unusual symptoms affecting your ears or balance.
Are Genetic Factors Significant in the Context of Hearing Loss?
Yes, genetic factors can contribute to hearing loss, and genetic testing may provide insights into hereditary conditions that affect auditory health.
Follow our journey on X!
The post Inner Ear vs. Outer Ear: Essential Differences Explained appeared first on The Microsuction Ear Wax Removal Network.
Originally posted 2025-04-21 03:11:44.
The post Inner Ear vs Outer Ear: Key Differences Uncovered appeared first on Healthcare Marketing Service.


