Last Updated on 10/10/2025 by Admin
In-Depth Exploration of Labyrinthitis: Understanding Its Impact
What Exactly is Labyrinthitis and How Does It Affect You?
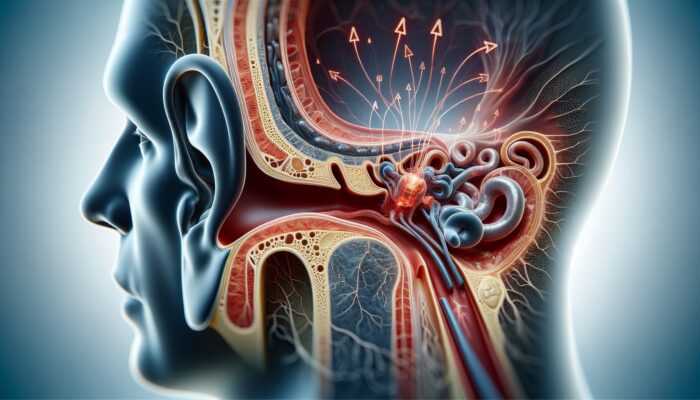
Labyrinthitis is a significant medical condition that impacts the inner ear, characterised by inflammation of the labyrinthine structure, which plays a vital role in maintaining balance and hearing. When inflammation disrupts the labyrinth’s normal functioning, it can lead to a variety of distressing symptoms that severely disrupt daily life. Many individuals experiencing labyrinthitis report distressing sensations, including:
- Dizziness
- Severe vertigo, a disorienting sensation of spinning
- Nausea and vomiting
- Hearing loss
- Tinnitus, often experienced as a persistent ringing in the ears
- Balance disturbances
- A general sense of unsteadiness
Labyrinthitis can manifest suddenly, leaving those affected feeling disoriented and anxious. This condition typically arises from an underlying infection or other health issues that provoke an immune response, resulting in symptoms that can significantly hinder daily activities and overall well-being.
What Are the Main Causes Contributing to Labyrinthitis?
Labyrinthitis can result from various causes, with the most common being viral or bacterial infections. Frequently encountered viral infections, such as the flu or upper respiratory infections, can lead to inflammation in the inner ear structure. In contrast, bacterial infections may develop from previous ear infections or sinusitis, allowing bacteria to migrate to the labyrinth. Furthermore, autoimmune responses can also trigger labyrinthitis when the immune system mistakenly attacks the inner ear tissues.
Understanding the underlying cause of labyrinthitis is paramount for effective treatment. For instance, if the origin is viral, healthcare providers may prescribe antiviral medications. Alternatively, a bacterial cause would necessitate the use of antibiotics. This comprehension is crucial for formulating the appropriate therapeutic approach tailored to the patient’s needs.
What Key Risk Factors Increase the Likelihood of Labyrinthitis?
Multiple factors can heighten the risk of developing labyrinthitis. A prominent risk factor includes a history of chronic ear infections, which may lead to ongoing inflammation and increase susceptibility to labyrinthitis. Individuals suffering from respiratory infections, especially those affecting the upper respiratory system, are also at an elevated risk, as these infections can spread to the inner ear.
Moreover, those with compromised immune systems, such as individuals living with HIV/AIDS or those undergoing chemotherapy, may face a higher likelihood of developing labyrinthitis. Additionally, individuals with a history of vestibular disorders or pre-existing ear issues should remain vigilant, as they may be more prone to this condition.
Identifying Symptoms and Diagnostic Techniques for Labyrinthitis
What Are the Most Common Symptoms Associated with Labyrinthitis?
The symptoms linked with labyrinthitis can be quite intense and vary in severity, ranging from mild discomfort to incapacitating episodes. Patients often report dizziness that can escalate into vertigo, resulting in a disorienting sensation of spinning, even while at rest. This experience of vertigo can lead to accompanying symptoms such as nausea and vomiting, further complicating the overall situation.
Hearing loss is another prevalent symptom, which can vary from temporary to permanent, contingent on the level of inflammation present. In conjunction with this, individuals may also experience tinnitus, which is characterised by a constant ringing or buzzing in the ears. These symptoms can profoundly disrupt daily life and negatively affect quality of life, underscoring the urgent need for timely medical assessment and intervention.
How is Labyrinthitis Accurately Diagnosed?
Diagnosing labyrinthitis requires a comprehensive approach that begins with a careful physical examination and an extensive review of the patient’s medical history. Healthcare professionals typically conduct hearing tests to assess auditory function, while balance assessments help ascertain the severity of the disorder.
Additionally, imaging studies such as MRI or CT scans may be employed to exclude other conditions and visualise the inner ear structures, focusing on any present abnormalities or inflammation. This thorough evaluation is vital for achieving an accurate diagnosis, enabling healthcare providers to devise targeted treatment strategies.
When Should You Seek Medical Attention for Labyrinthitis Symptoms?
It is crucial to seek immediate medical assistance if you experience symptoms such as sudden dizziness, severe vertigo, or hearing loss. These manifestations may indicate labyrinthitis or other serious conditions that require urgent care. Early diagnosis and treatment can significantly enhance outcomes, minimising the risk of long-term complications.
Prompt attention is essential, as untreated labyrinthitis can lead to more severe symptoms or complications, including permanent hearing loss. Patients who encounter persistent or worsening symptoms should not hesitate to consult healthcare professionals to ensure timely intervention.
How Can You Distinguish Labyrinthitis from Other Vestibular Disorders?
Labyrinthitis may often be confused with other vestibular disorders, such as Meniere’s disease or vestibular neuritis. Meniere’s disease is characterised by episodes of vertigo, hearing loss, and tinnitus, but it tends to involve more chronic symptoms and may present with fluctuating hearing loss. Conversely, vestibular neuritis primarily affects balance without the associated hearing loss that is typically observed in labyrinthitis.
A thorough evaluation is essential to differentiate labyrinthitis from these similar disorders. This usually involves a combination of patient history, symptom assessment, and diagnostic testing to identify the specific condition, which then informs appropriate treatment strategies.
What Can You Expect in Terms of Prognosis and Recovery from Labyrinthitis?
The prognosis for labyrinthitis can vary significantly among individuals. Most patients experience a gradual recovery within weeks, particularly when treated promptly and effectively. However, some individuals may continue to experience lingering symptoms, such as mild dizziness or balance issues, that could persist for months.
Timely treatment is crucial in improving recovery outcomes. Patients who receive swift medical attention and adhere to prescribed treatment regimens typically report more favourable recovery experiences, highlighting the importance of awareness and prompt action upon the onset of symptoms.
Examining Available Treatment Options for Labyrinthitis
What Medications Are Commonly Prescribed for Labyrinthitis Treatment?
Management of labyrinthitis generally begins by addressing its underlying cause, which may involve the use of various medications. In cases of viral infections, antiviral medications may be indicated, while bacterial infections usually necessitate antibiotics. In situations where inflammation is pronounced, corticosteroids can be administered to reduce swelling and alleviate symptoms.
Commonly prescribed medications for labyrinthitis include:
- Antivirals, such as acyclovir
- Antibiotics, like amoxicillin
- Corticosteroids, such as prednisone
- Antihistamines for relief from dizziness
- Anti-nausea medications, like meclizine
- Vestibular suppressants to alleviate vertigo symptoms
These medications aim to relieve symptoms while addressing the underlying inflammatory processes, guiding patients towards recovery.
What Advantages Does Vestibular Rehabilitation Offer for Labyrinthitis Patients?
Vestibular rehabilitation therapy (VRT) offers significant benefits for those experiencing balance issues related to labyrinthitis. This rehabilitative approach incorporates specific exercises designed to enhance balance, coordination, and reduce dizziness. By engaging in VRT, patients often experience transformative improvements in their overall quality of life.
Key benefits of vestibular rehabilitation include:
- Improved balance and stability
- Reduced frequency and intensity of dizziness episodes
- Enhanced coordination during daily activities
- Increased confidence in movement
Participants frequently find that these exercises not only alleviate symptoms but also empower them to manage their condition more effectively, fostering a sense of independence.
How Can Lifestyle Changes Enhance Management of Labyrinthitis?
In addition to medical treatments, adopting lifestyle changes can significantly influence the management of labyrinthitis symptoms. Stress reduction techniques, such as yoga or mindfulness, can help alleviate symptoms by decreasing overall tension in the body. Staying well-hydrated is also crucial, as dehydration can worsen dizziness and vertigo.
Moreover, avoiding substances like caffeine and alcohol can further assist in managing symptoms, as these can adversely affect inner ear function. Patients are encouraged to maintain a balanced diet rich in nutrients to support overall ear and body health, thereby enhancing their resilience against labyrinthitis symptoms.
Expert Insights on Labyrinthitis and Effective Management Strategies
What Perspectives Do Experts Offer Regarding Labyrinthitis?
Professionals in otolaryngology and neurology highlight the critical importance of early diagnosis and comprehensive management of labyrinthitis. A multidisciplinary approach, incorporating contributions from primary care physicians, otolaryngologists, and rehabilitation specialists, can optimise treatment outcomes.
For example, a case study involving a patient with labyrinthitis linked to a viral infection exemplifies the effectiveness of this coordinated approach. Following an initial diagnosis, the patient received antiviral medication alongside vestibular rehabilitation. Within weeks, they reported a marked reduction in dizziness and improved balance, demonstrating the value of prompt and collaborative care.
How Do Specialists Contribute to Labyrinthitis Treatment?
Specialists, such as otolaryngologists (ear, nose, and throat doctors) and neurologists, play a crucial role in diagnosing and treating labyrinthitis. Their expertise enables the creation of tailored treatment plans that address the specific needs of each patient and the root causes of labyrinthitis.
These specialists can provide targeted therapies, conduct advanced diagnostic testing, and guide patients through complex treatment protocols. Their partnership with primary care providers is essential to ensure a comprehensive approach, maximising recovery potential for those experiencing labyrinthitis.
What Are the Latest Research Developments in Labyrinthitis Treatment?
Recent investigations into labyrinthitis have focused on the role of inflammation and its impact on inner ear health. Studies suggest that understanding the mechanisms behind inflammation can aid in the development of new treatment options. For instance, researchers are exploring targeted therapies aimed at reducing inflammatory responses in the inner ear, which may lead to more effective labyrinthitis treatments in the future.
Additionally, research assessing the effectiveness of vestibular rehabilitation is highlighting its advantages for patients. Evidence indicates that personalised vestibular therapy can lead to improved balance and reduced symptom severity, reinforcing its integration into labyrinthitis treatment protocols.
What Symptoms Should You Be Aware of Regarding Labyrinthitis?
Common symptoms associated with labyrinthitis include vertigo, hearing loss, and tinnitus. Early recognition of these symptoms is crucial, as it can prompt timely medical evaluation and intervention. Individuals experiencing sudden bouts of dizziness or changes in hearing should seek medical attention, as these may indicate labyrinthitis or other serious conditions that require prompt care.
By understanding these symptoms, individuals can better manage their health and advocate for timely treatment, ultimately reducing the risk of long-term complications associated with labyrinthitis.
How Can Lifestyle Modifications Support Labyrinthitis Management?
Implementing lifestyle changes can greatly assist in managing labyrinthitis symptoms and enhancing overall well-being. Engaging in stress management techniques, such as mindfulness and yoga, can alleviate anxiety and promote a sense of calm. Ensuring proper hydration and nutrition supports the body’s healing processes and bolsters ear health.
Moreover, individuals should aim to avoid common triggers like caffeine and alcohol, as these substances can exacerbate symptoms. By prioritising self-care and implementing thoughtful lifestyle adjustments, patients can improve their ability to manage labyrinthitis symptoms, leading to a better quality of life.
Effective Strategies for Coping with Labyrinthitis
How Can You Successfully Manage Daily Life While Living with Labyrinthitis?
Living with labyrinthitis can present numerous challenges, yet implementing effective strategies can significantly ease daily life. Utilising assistive devices, such as canes or walkers, can provide essential support during episodes of dizziness and unsteadiness.
Adjusting your living environment for safety is vital; for instance, removing tripping hazards and installing grab bars in bathrooms can mitigate fall risks. Additionally, seeking social support from friends, family, or local support groups can enhance emotional well-being, allowing patients to share their experiences and coping mechanisms.
Practical steps for managing daily life with labyrinthitis include:
- Utilising assistive walking devices when necessary.
- Creating a secure home environment by eliminating hazards.
- Maintaining consistent communication with healthcare providers.
- Joining support groups or online communities for emotional support.
By taking these proactive measures, individuals living with labyrinthitis can navigate daily activities with greater confidence and safety.
What Advantages Do Support Networks Offer to Labyrinthitis Patients?
Joining support networks can provide invaluable resources for patients coping with labyrinthitis. Support groups, whether in-person or online, offer emotional assistance and a platform for sharing experiences. These communities foster an environment of understanding, where individuals can discuss coping strategies and treatment options.
Patients benefit from learning about others’ experiences, discovering tips for symptom management, and receiving encouragement during challenging times. This sense of camaraderie can significantly enhance emotional resilience, making the journey with labyrinthitis feel less isolating.
What Psychological Effects Can Labyrinthitis Induce?
Labyrinthitis can lead to various psychological impacts, including anxiety, depression, and a heightened fear of falling. The unpredictable nature of symptoms can instil feelings of helplessness and insecurity in patients, adversely affecting their mental health and overall quality of life.
Addressing these psychological effects is essential for comprehensive care. Engaging in cognitive-behavioural therapy or counselling can equip patients with coping strategies to manage anxiety and fear effectively. Additionally, support from family and friends fosters a positive environment, encouraging patients to express their feelings and seek help when necessary.
Preventative Strategies and Long-Term Management of Labyrinthitis
Can Labyrinthitis Be Effectively Prevented?
While not all cases of labyrinthitis are preventable, certain proactive measures can significantly reduce risk. Maintaining good ear health is essential; this entails seeking prompt treatment for ear infections and practising proper hygiene to minimise the likelihood of respiratory infections.
Moreover, individuals with chronic health conditions should manage these effectively, as they can contribute to the development of labyrinthitis. Regular check-ups with healthcare providers can facilitate early detection and management of conditions that may predispose individuals to labyrinthitis.
What Are the Long-Term Management Strategies for Labyrinthitis?
Long-term management of labyrinthitis necessitates a comprehensive approach that includes consistent follow-ups with healthcare providers. Patients may benefit from ongoing vestibular rehabilitation to strengthen balance and coordination.
Furthermore, implementing lifestyle changes such as stress management, proper hydration, and a nutritious diet can significantly enhance overall health and resilience against labyrinthitis symptoms. Regular evaluations by specialists help to tailor management strategies to meet individual needs and prevent recurrence.
What Lifestyle Adjustments Are Beneficial for Managing Labyrinthitis?
Lifestyle modifications play a crucial role in managing labyrinthitis symptoms and improving overall health. Engaging in regular exercise tailored to personal abilities can enhance balance and coordination. A balanced diet rich in nutrients supports bodily functions and strengthens the immune system.
Stress management strategies, including mindfulness practices or yoga, can greatly reduce symptoms and improve emotional well-being. Prioritising adequate sleep is also vital, as restorative sleep is essential for recovery and resilience against labyrinthitis-related symptoms.
Understanding Complications and Associated Conditions of Labyrinthitis
What Potential Complications Can Arise from Labyrinthitis?
Complications arising from labyrinthitis can include permanent hearing loss, chronic dizziness, and an increased risk of falls. Awareness of these risks is vital for patients and caregivers, as they underscore the importance of early intervention and effective management strategies.
Patients must remain vigilant and report any unusual changes in symptoms to their healthcare providers. Comprehensive care, which encompasses regular follow-ups and proactive symptom management, can help mitigate these complications effectively.
How Does Labyrinthitis Differ from Meniere’s Disease?
Labyrinthitis and Meniere’s disease share similar symptoms, such as vertigo, tinnitus, and hearing loss. However, they are distinct conditions with different underlying causes. Meniere’s disease typically involves episodic symptoms associated with fluid accumulation in the inner ear, while labyrinthitis primarily results from inflammation.
Understanding these differences is crucial for accurate diagnosis and treatment. Patients experiencing symptoms should undergo thorough evaluations to determine the underlying condition and receive appropriate care to ensure effective management.
Which Other Conditions Can Mimic Labyrinthitis Symptoms?
Several conditions may present symptoms akin to labyrinthitis, including vestibular neuritis, benign paroxysmal positional vertigo (BPPV), and migraines. Vestibular neuritis primarily affects balance and does not typically involve hearing loss, while BPPV occurs due to dislodged calcium crystals in the inner ear, resulting in positional vertigo.
A comprehensive evaluation is necessary to differentiate these disorders from labyrinthitis. Accurate diagnosis ensures that patients receive the most effective treatment for their specific condition, ultimately leading to improved recovery outcomes.
Proven Strategies for Understanding and Treating Labyrinthitis
What Are the Most Effective Treatment Strategies for Labyrinthitis?
Effective treatment strategies for labyrinthitis involve a multifaceted approach that integrates medications, vestibular rehabilitation, and lifestyle modifications. Tailoring these strategies to individual patient needs is essential for achieving optimal outcomes.
Medications targeting the underlying cause, such as antivirals or antibiotics, are crucial for addressing inflammation. Vestibular rehabilitation exercises aim to enhance balance and reduce dizziness, while lifestyle changes reinforce overall health and resilience against symptoms.
Expert analysis suggests that a combination of these strategies yields the best results, enabling patients to regain their quality of life while effectively managing labyrinthitis.
How Can You Personalise Treatment to Meet Your Specific Needs?
Customising treatment for labyrinthitis necessitates close collaboration with healthcare providers to develop a personalised plan. This plan should consider the specific symptoms, underlying causes, and individual health conditions of the patient.
Regular communication with healthcare professionals allows for adjustments based on treatment effectiveness and symptom progression. This collaborative approach ensures that patients receive the best possible care, enhancing their chances for a successful recovery.
What Role Does Patient Education Play in Labyrinthitis Management?
Patient education is critical for effective management of labyrinthitis. Understanding the condition, its symptoms, and available treatment options empowers patients to engage actively in their care. Informed patients are more likely to adhere to treatment plans, recognise changes in symptoms, and seek timely medical assistance when necessary.
Moreover, educating patients about lifestyle modifications and preventative measures can empower them to take control of their health, ultimately leading to improved outcomes and enhanced quality of life in managing labyrinthitis.
Future Directions in Labyrinthitis Research and Treatment
What Does the Future Hold for Labyrinthitis Treatment Innovations?
The future of labyrinthitis treatment appears promising, with ongoing research focused on developing targeted therapies and advanced diagnostic tools. Innovations in treatment methods could lead to more effective interventions that address the underlying causes of labyrinthitis, particularly in cases linked to inflammation.
As our understanding of labyrinthitis evolves, the formulation of personalised treatment plans based on individual patient profiles is expected to enhance recovery outcomes and improve the quality of life for those affected by this condition.
How Is Technology Enhancing Labyrinthitis Treatment?
Technological advancements play a pivotal role in improving the diagnosis and treatment of labyrinthitis. For example, virtual reality technology is being incorporated into vestibular rehabilitation programmes, providing immersive environments for patients to engage in balance exercises.
Additionally, advanced imaging techniques, such as high-resolution MRI, facilitate more accurate assessments of inner ear structures, enabling earlier diagnosis and better treatment planning. These technological innovations are poised to transform the landscape of labyrinthitis management.
What Are the Current Research Priorities in Labyrinthitis?
Current research priorities for labyrinthitis focus on elucidating the underlying mechanisms of the condition, exploring new treatment modalities, and enhancing patient care. Investigating the inflammatory processes contributing to labyrinthitis is essential for developing targeted therapies that can alleviate symptoms and prevent recurrence.
Moreover, research aims to improve vestibular rehabilitation techniques to maximise their effectiveness and ensure patient adherence. This ongoing inquiry is vital for advancing our understanding of labyrinthitis and improving the lives of those affected.
How Can Labyrinthitis Research Benefit Other Vestibular Disorders?
Research on labyrinthitis holds the potential to provide significant insights for understanding and treating other vestibular disorders. By unraveling the mechanisms underlying labyrinthitis, researchers may identify common pathways and treatment strategies applicable to a variety of conditions, such as vestibular neuritis and Meniere’s disease.
This interconnectedness among vestibular disorders underscores the importance of comprehensive research efforts that could lead to breakthroughs in care and rehabilitation strategies across a range of conditions affecting balance and hearing.
Frequently Asked Questions About Labyrinthitis and Its Management
What is labyrinthitis?
Labyrinthitis is an inner ear disorder characterised by inflammation of the labyrinth, which affects balance and hearing, often resulting in symptoms such as dizziness and vertigo.
What causes labyrinthitis?
Labyrinthitis can arise from viral infections, bacterial infections, and autoimmune responses, with comprehending the underlying cause being essential for effective treatment.
What are the common symptoms of labyrinthitis?
Common symptoms include dizziness, vertigo, nausea, hearing loss, and tinnitus, varying in severity and impacting daily life.
How is labyrinthitis diagnosed?
Diagnosis typically involves a thorough physical examination, hearing tests, balance tests, and imaging studies to rule out other conditions.
When should I seek medical attention for labyrinthitis?
You should seek medical assistance if you experience sudden dizziness, vertigo, or hearing loss, as early diagnosis can significantly improve outcomes.
What are the treatment options for labyrinthitis?
Treatment options may include medications such as antivirals and antibiotics, vestibular rehabilitation, and lifestyle changes to manage symptoms effectively.
Can labyrinthitis be prevented?
While not all cases can be prevented, maintaining good ear health, promptly treating infections, and managing underlying conditions can reduce the risk of labyrinthitis.
What role does lifestyle play in managing labyrinthitis?
Lifestyle adjustments, including stress reduction, hydration, and a balanced diet, can significantly aid in managing labyrinthitis symptoms and improving overall quality of life.
What are the potential complications of labyrinthitis?
Potential complications include permanent hearing loss, chronic dizziness, and an increased risk of falls, underscoring the importance of early intervention and management.
How can I cope with daily life while living with labyrinthitis?
Coping strategies include using assistive devices, modifying your environment for safety, and seeking support from friends, family, or support groups to enhance emotional well-being.
Explore our world on X!
The post Labyrinthitis: Understanding and Treating the Condition appeared first on The Microsuction Ear Wax Removal Network.
The post Labyrinthitis: Understanding and Treating the Condition appeared first on Healthcare Marketing Service.